This Framingham risk score calculator estimates the 10-year coronary heart disease risk of any person based on certain criteria like. The Framingham Risk Calculator shows your risk of heart disease, using your cholesterol values, blood pressure, gender. The result is a risk score. This Framingham risk score calculator estimates the 10-year coronary heart disease risk of any person based on certain criteria like gender, age, cholesterol and systolic pressure. You can discover more about this heart disease scoring system and about all the cardiovascular risk factors involved below the form.
Contents. Cardiovascular Risk Scoring systems The Framingham Risk Score is one of a number of scoring systems used to determine an individual's chances of developing cardiovascular disease. A number of these scoring systems are available online. Cardiovascular risk scoring systems give an estimate of the probability that a person will develop cardiovascular disease within a specified amount of time, usually 10 to 30 years.
Because they give an indication of the risk of developing cardiovascular disease, they also indicate who is most likely to benefit from prevention. For this reason, cardiovascular risk scores are used to determine who should be offered preventive drugs such as drugs to lower blood pressure and drugs to lower cholesterol levels. For example, nearly 30% of coronary heart disease (CHD) events in both men and women were singularly attributable to blood pressure levels that exceeded high normal (≥130/85), showing that blood pressure management and monitoring is paramount both to cardiovascular health and prediction of outcomes. Usefulness Because risk scores such as the Framingham Risk Score give an indication of the likely benefits of prevention, they are useful for both the individual patient and for the clinician in helping decide whether lifestyle modification and preventive medical treatment, and for patient education, by identifying men and women at increased risk for future cardiovascular events. (CHD) risk at 10 years in percent can be calculated with the help of the Framingham Risk Score. Individuals with low risk have 10% or less CHD risk at 10 years, with intermediate risk 10-20%, and with high risk 20% or more. However it should be remembered that these categorisations are arbitrary.
A more useful metric is to consider the effects of treatment. If a group of 100 persons all have a 20% ten-year risk of cardiovascular disease it means that we should expect that 20 of these 100 individuals will develop cardiovascular disease (coronary heart disease or stroke) in the next 10 years and eighty of them will not develop cardiovascular disease in the next 10 years. If they were to take a combination of treatments (for example drugs to lower cholesterol levels plus drugs to lower blood pressure) that reduced their risk of cardiovascular disease by half it means that 10 of these 100 individuals should be expected to develop cardiovascular disease in the next 10 years and 90 of them should not be expected to develop cardiovascular disease. If that was the case then 10 of these individuals would have avoided cardiovascular disease by taking treatment for 10 years; 10 would get cardiovascular disease whether or not they took treatment; and 80 would not have got cardiovascular disease whether or not they took treatment. Despite their widespread popularity, randomised trials assessing the impact of using cardiovascular disease risk scores show limited impact on patient outcomes.
Although there is good evidence that targeting individuals with high total CVD risk is the most efficient way to reduce CVD-related morbidity and mortality, to date trials assessing the usefulness of risk scores at helping clinicians target high risk patients show limited benefit. Issues Raised by Cardiovascular Risk Prediction It is important to recognize that the strongest predictor of cardiovascular risk in any risk equation is age. Almost all persons aged 70 and over are at 20% ten year cardiovascular risk and almost nobody aged under 40 is at 20% ten year cardiovascular risk. Since those who benefit most from treatment are those at highest risk, this means that treatment of patients with raised blood pressure and raised cholesterol levels in their thirties benefits very few. Whereas treatment of patients with 'normal' blood pressure and 'normal' cholesterol levels in their seventies benefits many. This casts doubt on the wisdom of categorizing individuals as having high blood pressure or raised cholesterol and treating these individual risk factors without a consideration of both their overall risk of cardiovascular disease and of the probability that they will benefit. Background is common in the general population, affecting the majority of adults.
It includes: 1) (CHD): (MI), (HF), and. 2), and (TIA). 3), and significant limb. 4) Aortic disease: Aortic, and. An individual’s risk for future cardiovascular events is modifiable, by lifestyle changes and preventive medical treatment.
Lifestyle changes can include stopping, regular, etc. Preventive medical treatment can include a, mini dose, treatment for, etc. It is important to be able to predict the risk of an individual patient, in order to decide when to initiate lifestyle modification and preventive medical treatment. Multiple risk models for the prediction of cardiovascular risk of individual patients have been developed. One such key is the Framingham Risk Score. The Framingham Risk Score is based on findings from the. Validation The Framingham Risk Score has been validated in the USA, both in men and women, both in European Americans and African Americans.
While several studies have claimed to improve on the FRS, there is little evidence for any improved prediction beyond the Framingham risk score Limitations There are two limitations. The Framingham Risk Score predicts only future coronary heart disease (CHD) events, however, it does not predict future total cardiovascular events, meaning that it does not predict risk for stroke, transient ischemic attack (TIA), and heart failure. These also important patient outcomes were included in the 2008 Framingham General Cardiovascular Risk Score. The predicted risk for an individual usually is higher with the 2008 Framingham General Cardiovascular Risk Score than with the 2002 Framingham Risk Score.

The Framingham Risk Score could overestimate (or underestimate) risk in populations other than the US population, and within the USA in populations other than European Americans and African Americans, e.g. Hispanic Americans and Native Americans. It is not yet clear if this limitation is real, or appears to be real because of differences in methodology, etc. As a result, other countries may prefer to use another risk score, e.g. (HeartScore is the interactive version of SCORE - Systematic COronary Risk Evaluation), which has been recommended by the in 2007.
If possible, a professional should select the risk prediction model which is most appropriate for an individual patient and should remember that this is only an estimate. Versions The current version of the Framingham Risk Score was published in 2008. The publishing body is the ATP III, i.e.
The «Adult Treatment Panel III», an expert panel of the, which is part of the (NIH), USA. The prior version was published in 2002 The original Framingham Risk Score had been published in 1998. Differences between the versions The first Framingham Risk Score included age, sex, LDL cholesterol, HDL cholesterol, blood pressure (and also whether the patient is treated or not for his/her hypertension), diabetes, and smoking.
It estimated the 10-year risk for coronary heart disease (CHD). It performed well, and correctly predicted 10-year risk for CHD in American men and women of European and African descent. The updated version was modified to include, age range, hypertension treatment, smoking, and total cholesterol, and it excluded, because Type 2 diabetes meanwhile was considered to be a CHD Risk Equivalent, having the same 10-year risk as individuals with prior CHD. Patients with Type 1 diabetes were considered separately with slightly less aggressive goals; while at increased risk, no study had shown them to be at equivalent risk for CHD as those with previously diagnosed coronary disease or Type 2 diabetes.
CHD Risk Equivalent Some patients without known CHD have risk of cardiovascular events that is comparable to that of patients with established CHD. Cardiology professionals refer to such patients as having a CHD risk equivalent. These patients should be managed as patients with known CHD. CHD risk equivalents are patients with a 10-year risk for or 20%. CHD risk equivalents are primarily other clinical forms of atherosclerotic disease.
The NCEP's ATP III guidelines also list diabetes as a CHD risk equivalent since it also has a 10-year risk for CHD around 20%. NCEP ATP III CHD risk equivalents are:. clinical (CHD). symptomatic (CAD). (PAD). (AAA).
Analysis of the US population with the Framingham/ATP III criteria The Framingham/ATP III criteria were used to estimate CHD risk in the USA. Data from 11,611 patients from a very large study, the III, were used.
The patients were 20 to 79 years of age, and had no self reported CHD, stroke, peripheral arterial disease, or diabetes. The results: 82% of patients had low risk (10% or less CHD risk at 10 years). 16% had intermediate risk (10-20%). 3% had high risk (20% or more). High risk was most commonly found in patients with advanced age, and was more common in men than women. High risk patients are sometimes become unknown with certain signs and symptoms of cardiac failure Scoring Framingham Risk Score for Women Age: 20–34 years: Minus 7 points. 35–39 years: Minus 3 points.
40–44 years: 0 points. 45–49 years: 3 points. 50–54 years: 6 points. 55–59 years: 8 points. 60–64 years: 10 points. 65–69 years: 12 points. 70–74 years: 14 points.
75–79 years: 16 points. Total cholesterol, mg/dL: Age 20–39 years: Under 160: 0 points. 160-199: 4 points.
200-239: 8 points. 240-279: 11 points.
280 or higher: 13 points. Age 40–49 years: Under 160: 0 points. 160-199: 3 points. 200-239: 6 points. 240-279: 8 points. 280 or higher: 10 points.
Age 50–59 years: Under 160: 0 points. 160-199: 2 points. 200-239: 4 points. 240-279: 5 points.
280 or higher: 7 points. Age 60–69 years: Under 160: 0 points. 160-199: 1 point. 200-239: 2 points. 240-279: 3 points. 280 or higher: 4 points.
Age 70–79 years: Under 160: 0 points. 160-199: 1 point. 200-239: 1 point. 240-279: 2 points. 280 or higher: 2 points. If cigarette smoker: Age 20–39 years: 9 points. Age 40–49 years: 7 points.
Age 50–59 years: 4 points. Age 60–69 years: 2 points. Age 70–79 years: 1 point.
All non smokers: 0 points. HDL cholesterol, mg/dL: 60 or higher: Minus 1 point. 50-59: 0 points. 40-49: 1 point.
Under 40: 2 points. Systolic blood pressure, mm Hg: Untreated: Under 120: 0 points. 120-129: 1 point. 130-139: 2 points. 140-159: 3 points. 160 or higher: 4 points.
Treated: Under 120: 0 points. 120-129: 3 points. 130-139: 4 points. 140-159: 5 points.
160 or higher: 6 points. 10-year risk in%: Points total: Under 9 points: 25= Over 30% Framingham Risk Score for Men Age: 20–34 years: Minus 9 points. 35–39 years: Minus 4 points.
40–44 years: 0 points. 45–49 years: 3 points. 50–54 years: 6 points. 55–59 years: 8 points.
60–64 years: 10 points. 65–69 years: 11 points. 70–74 years: 12 points.
75–79 years: 13 points. Total cholesterol, mg/dL: Age 20–39 years: Under 160: 0 points. 160-199: 4 points. 200-239: 7 points. 240-279: 9 points. 280 or higher: 11 points.
Age 40–49 years: Under 160: 0 points. 160-199: 3 points. 200-239: 5 points. 240-279: 6 points.
280 or higher: 8 points. Age 50–59 years: Under 160: 0 points. 160-199: 2 points. 200-239: 3 points. 240-279: 4 points.
280 or higher: 5 points. Age 60–69 years: Under 160: 0 points. 160-199: 1 point. 200-239: 1 point. 240-279: 2 points.
280 or higher: 3 points. Age 70–79 years: Under 160: 0 points. 160-199: 0 points. 200-239: 0 points. 240-279: 1 point. 280 or higher: 1 point.
If cigarette smoker: Age 20–39 years: 8 points. Age 40–49 years: 5 points. Age 50–59 years: 3 points. Age 60–69 years: 1 point.
Age 70–79 years: 1 point. All non smokers: 0 points. HDL cholesterol, mg/dL: 60 or higher: Minus 1 point. 50-59: 0 points.
40-49: 1 point. Under 40: 2 points.
Systolic blood pressure, mm Hg: Untreated: Under 120: 0 points. 120-129: 0 points. 130-139: 1 point. 140-159: 1 point. 160 or higher: 2 points. Treated: Under 120: 0 points.
120-129: 1 point. 130-139: 2 points. 140-159: 2 points. 160 or higher: 3 points. 10-year risk in%: Points total: 0 point.
P.W., Wilson; D'Agostino, R.B.; Levy, D.; Belanger, A.M.; Silbershatz, H.; Kannel, W.B. (12 May 1998). 97 (18): 1837–1847.
Retrieved 7 May 2013. D'Agostino, R.B.; Vasan, R.S.; Pencina, M.J.; Wolf, P.A.; Cobain, M.; Massaro, J.M.; Kannel, W.B. (22 January 2008). 'General cardiovascular risk profile for use in primary care: the Framingham Heart Study'. 117 (6): 743–753. Collins, Dylan; Lee, Joseph; Bobrovitz, Niklas; Koshiaris, Constantinos; Ward, Alison; Heneghan, Carl (2016-10-14).
Retrieved 2013-09-14. Framingham Heart Study. Retrieved 7 May 2013. Wilson, PW; D'Agostino, RB; Levy, D; Belanger, AM; Silbershatz, H; Kannel, WB (1998). 'Prediction of coronary heart disease using risk factor categories'.
Oct 18, 2015 - 6 min - Uploaded by brasstaxPoni Hoax LP, Tigersushi Records. Jun 9, 2010 - 5 min - Uploaded by Emmanuel CamaitiFrom Poni Hoax - Budapest EP Label: Tigersushi TSR 017 Format: Vinyl, 12', EP, 45 RPM. May 1, 2010 - 7 min - Uploaded by cineversity.tvIt was crazy, we filmed this French band, a sort of French Talking Heads, but this time they. Nicolas Villebrun.
97 (18): 1837–47. Estimation of cardiovascular risk in an individual patient without known cardiovascular disease. In: UpToDate Textbook of Medicine. Basow, DS (Ed). Massachusetts Medical Society, and Wolters Kluwer publishers, The Netherlands. Collins, Dylan Raymond James; Tompson, Alice; Onakpoya, Igho; Roberts, Nia; Ward, Alison; Heneghan, Carl (2017). 'Global cardiovascular risk assessment in the primary prevention of cardiovascular disease in adults: systematic review of systematic reviews'.
Validation of the Framingham coronary heart disease prediction scores: results of a multiple ethnic groups investigation. D'Agostino RB Sr, Grundy S, Sullivan LM, Wilson P. 2001 Jul 11;286(2):180-7. Tzoulaki, I.; Liberopoulos, G.; Ioannidis, JP. 'Assessment of claims of improved prediction beyond the Framingham risk score'. 302 (21): 2345–52.
D'Agostino RB Sr; Vasan RS; Pencina MJ; Wolf PA; Cobain M; Massaro JM; Kannel WB (Feb 2008). 'General cardiovascular risk profile for use in primary care: the Framingham Heart Study'. 117 (6): 743–53. Brindle P, Emberson J, Lampe F, Walker M, Whincup P, Fahey T, Ebrahim S (Nov 2003). 327 (7426): 1267. Liu J; Hong Y; D'Agostino RB Sr; Wu Z; Wang W; Sun J; Wilson PW; Kannel WB; Zhao D (Jun 2004).
'Predictive value for the Chinese population of the Framingham CHD risk assessment tool compared with the Chinese Multi-Provincial Cohort Study'. 291 (21): 2591–9. Sacco RL, Khatri M, Rundek T, Xu Q, Gardener H, Boden-Albala B, Di Tullio MR, Homma S, Elkind MS, Paik MC (Dec 2009). 'Improving global vascular risk prediction with behavioral and anthropometric factors. The multiethnic NOMAS (Northern Manhattan Cohort Study)'. J Am Coll Cardiol. 54 (24): 2303–11.
Estimation of ten-year risk of fatal cardiovascular disease in Europe: the SCORE project European Heart Journal 2003;24:987-1003. Conroy RM, Pyorala K, Fitzgerald AP, Sans S, Menotti A, De Backer G, De Bacquer D, Ducimetiere P, Jousilahti P, Keil U, Njolstad I, Oganov RG, Thomsen T, Tunstall-Pedoe H, Tverdal A, Wedel H, Whincup P, Wilhelmsen L, Graham IM (Jun 2003). 'Estimation of ten-year risk of fatal cardiovascular disease in Europe: the SCORE project'.
24 (11): 987–1003. ^ Third Report of the National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III) final report. 2002 Dec 17;106(25):3143-421. Prediction of coronary heart disease using risk factor categories. Wilson PW, D'Agostino RB, Levy D, Belanger AM, Silbershatz H, Kannel WB. 1998 May 12;97(18):1837-47. The distribution of 10-Year risk for coronary heart disease among US adults: findings from the National Health and Nutrition Examination Survey III.
Ford ES, Giles WH, Mokdad AH. J Am Coll Cardiol. 2004 May 19;43(10):1791-6. Retrieved 2013-09-14. Development of a risk score for atrial fibrillation (Framingham Heart Study): a community-based cohort study.
Schnabel RB, Sullivan LM, Levy D, Pencina MJ, Massaro JM, D'Agostino RB Sr, Newton-Cheh C, Yamamoto JF, Magnani JW, Tadros TM, Kannel WB, Wang TJ, Ellinor PT, Wolf PA, Vasan RS, Benjamin EJ. 2009 Feb 28;373(9665):739-45. Lifetime risk for development of atrial fibrillation: the Framingham Heart Study. Lloyd-Jones DM, Wang TJ, Leip EP, Larson MG, Levy D, Vasan RS, D'Agostino RB, Massaro JM, Beiser A, Wolf PA, Benjamin EJ. 2004 Aug 31;110(9):1042-6.
Abstract The prevalence and burden of cardiovascular disease (CVD) is high, and it remains the leading cause of death worldwide. Unfortunately, many individuals who are at high risk for CVD are not recognized and/or treated. Therefore, programs are available to ensure individuals at risk for CVD are identified through appropriate risk classification and offered optimal preventative interventions. The use of algorithms to determine a global risk score may help to achieve these goals. Such global risk-scoring algorithms takes into account the synergistic effects between individual risk factors, placing increases in individual risk factors into context relative to the overall disease, allowing for a continuum of disease risk to be expressed, and identifying patients most likely to derive benefit from an intervention.
The predictive value of risk scoring such as using the Framingham equation is reasonable, analogous to cervical screening, with area under the receiver operated characteristic curve a little over 70%. However, limitations do exist, and as they are identified adjustments can be made to the global risk-scoring algorithms. Limitations include patient-specific issues, such as variations in lifetime risk level, ethnicity or socio-economic strata, and algorithm-specific issues, such as discrepancies between different algorithms arising from varying risk factors evaluated. The use of currently developed algorithms is low in general practice, in part, because of the belief that the assessment may oversimplify the risk and/or lead to medication overuse. Additional hindrances to the use of risk scoring include government or local health policy, patient compliance issues and lack of time.
A thorough, easy-to-use, and standardized tool for risk estimation would allow for improvements in the primary prevention of CVD. Introduction Cardiovascular disease (CVD) is the leading cause of death worldwide. The major risk factors for CVD are well established, with the principal three modifiable factors being hypertension, dyslipidemia and smoking. Studies have shown that between 81% and 92% of the patients with coronary heart disease (CHD) have at least one of these three risk factors, and each has a continuous dose-dependent effect on CHD risk., Although some risk factors, such as age and genetic profile, are not modifiable, most others, including high blood pressure, elevated cholesterol, poor diet, obesity, smoking, stress and inactivity, are amenable to intervention. Development of evidence-based treatment guidelines and implementation programs to facilitate the prevention and treatment of CVD is a priority in many countries.
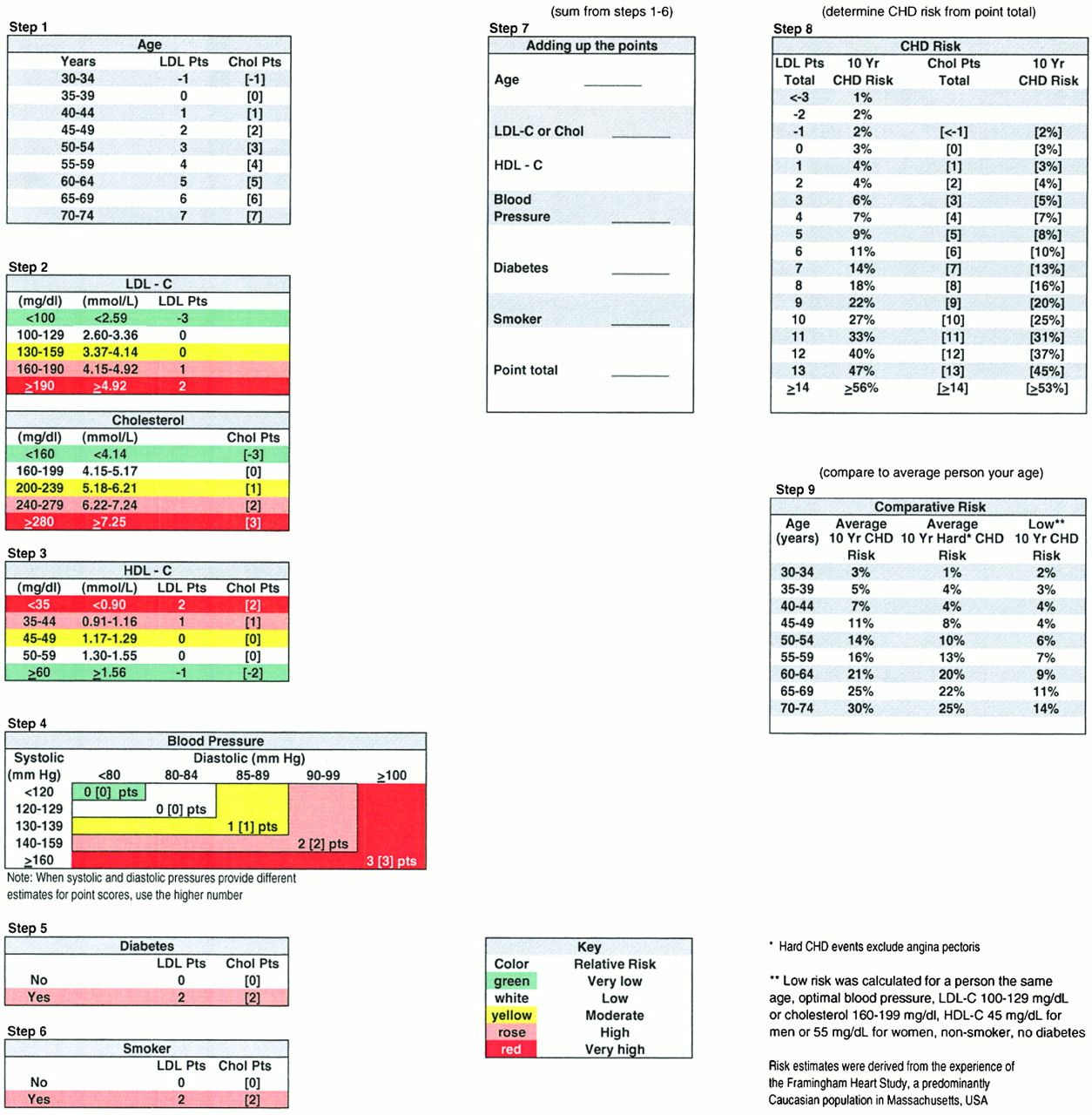
Framingham Risk Score Chart
Several large clinical outcome studies have demonstrated that CVD morbidity and mortality can be significantly reduced by the adoption of healthy lifestyle changes and the use of anti-hypertensive and lipid-lowering agents, especially statins. Evidence has also accumulated to guide how intensively patients should be treated according to their CVD risk.
These results reinforce the importance of treating patients with established CVD and also highlight the increasing importance of identifying patients at risk and treating them prior to the development of CVD. Despite the enormous burden of CVD, many patients remain undiagnosed and untreated. Even among patients with established disease, there are substantial treatment gaps; among patients receiving lipid-modifying therapy, 43% do not achieve total cholesterol targets (90% of the family physicians screened adults for hyperlipidemia as part of a CVD prevention strategy; most physicians (85%) were aware of the National Cholesterol Education Program (NCEP) Adult Treatment Panel (ATP) III guidelines, but only 13% had read them carefully and only 17% usually or always used a CHD risk calculator. The authors concluded that there existed ‘a large variability in knowledge, beliefs, and practice patterns among practicing family physicians’. A survey of 26 general practitioners (GPs) in Germany that evaluated the primary prevention of CVD confirmed that in general neither guidelines nor risk calculators were used.
Framingham Risk Calculator Pdf
Seventy-five percent of GPs used a high-risk strategy in primary prevention, but ∼50% admitted to not using guidelines, and 70% did not use risk calculators. Physicians treatment decisions were influenced by factors such as patient values or wishes as well as the healthcare system. A survey conducted by the European Society of Cardiology in six European countries helps to explain why many physicians rely on their own expertise for the prevention and treatment of CHD. Although the majority of cardiologists and physicians (85%) who participated in this survey were aware of the need to base CVD risk assessments on the combination of all CVD risk factors, 62% of physicians used subjective methods to gage risk rather than guidelines or risk calculators. The most common barriers to guideline implementation were government or local health policy (40%), patient compliance (36%) and lack of time (23%). Various suggestions were proposed to improve implementation including development of clear, easy to use and simpler guidelines (prompted = 46%; unprompted = 23%) and greater financial incentives (unprompted = 24%).
Although preferred by many physicians, intuitive assessment based on personal experience appears to underestimate the real risk of CVD. A study conducted in Sweden investigated differences between recommendations presented in the 1999 World Health Organization–International Society of Hypertension (WHO/ISH) Guidelines and doctors' risk estimation and willingness to prescribe antihypertensive medications. Physicians (110 GPs and 29 specialists in internal medicine or cardiology) estimated CVD risk as being less severe than recommendations provided in the WHO/ISH guidelines.
Moreover, physicians’ willingness to prescribe antihypertensive medications was inferior to guideline recommendations. Specialists were more inclined to prescribe antihypertensive medications than GPs.
The European guidelines recommend total CVD assessments when certain risk factors are present, and a summary of recommendations for assessing CVD is presented in. Summary of recommendations for total CVD assessment in clinical practice.
BP: Blood pressure; HR: Heart rate; LDL: Low-density lipoprotein; HDL: High-density lipoprotein; ECG: Electrocardiogram; CRP: C-reactive protein; DM: Diabetes mellitus; BMI: Body mass index; WC: Waist circumference; TC: Total cholesterol. Reprinted with permission from Graham et al. Nurses play a key role in the prevention of CVD; however, similar to physicians, nurses also have a tendency to inaccurately estimate CVD risk. Two hundred and eighty-seven participants at a European conference of cardiovascular nursing were asked to complete questionnaires to assess their own CVD risk and to estimate their absolute risk of experiencing a fatal CVD event within 10 years. Most nurses poorly understood their own CVD risk profile; less than half of the nurse’s self-reported 10-year risk of a fatal CVD event (46%) corresponded with their CVD risk calculated using SCORE. Improvements need to be implemented so that healthcare providers develop an accurate perception of CVD risk assessment.
A thorough and easy to accomplish risk estimation is essential, as was demonstrated by a study of 500 physicians (300 primary care physicians, 100 obstetricians/gynecologists and 100 cardiologists), where perception of risk was the primary driver of CVD preventative recommendations. Limitations of risk scoring Global CVD risk scores attempt to predict the likelihood of CVD events with reasonable accuracy in a broad patient population.